I’ve been symptomatic all my life, but didn’t always know it. Of what, you ask?
Bipolar disorder
Bipolar disorder is a mental illness characterized by periods of depression alternating with at least one period of mania or hypomania. It comes in three forms: Bipolar I, Bipolar II and Cyclothymia.
Bipolar I – This is classic “manic depression”—a state of mania (high energy, arousal and/or elation, anger, irritability, hostility and potentially psychosis) punctuated by depression (sadness, hopelessness, despair, feelings of worthlessness and pessimism about the future, and again, potentially psychosis).
Bipolar II – In this form, depression alternates with hypomania, a less intense but still debilitating form of mania.
Cyclothymia – With this form, you’ll have depression akin to dysthymia (low-grade depression), along with hypomania and/or mixed states, and you may experience rapid cycling between these moods.
Only about 2 percent of Canadians are struggling with bipolar disorder, but 20 percent of the population will face mental illness at some point in their lives, and only 7 percent of Canada’s medical funding goes to mental health—lending gravitas to the new CAMH (Centre for Addiction and Mental Health) Foundation campaign—“mental health is health.”
My brain vs. your brain
 What people don’t understand about mental illness is the nature versus nurture aspect. Often you hear “pull up your bootstraps,” as if mental illness were the result of laziness or maladaptive coping mechanisms; and some people will give you the benefit of the doubt of genetics.
What people don’t understand about mental illness is the nature versus nurture aspect. Often you hear “pull up your bootstraps,” as if mental illness were the result of laziness or maladaptive coping mechanisms; and some people will give you the benefit of the doubt of genetics.
But while maladaptive coping mechanisms are the linchpin of “neurotic” conditions, differing brain anatomy underlies most “psychotic” conditions.
In the same way that I may differ from you in height or shoe size, my brain differs from yours in its physical structure and function. We think differently because we have fundamentally different brains, not just because I think “incorrectly.” And it has nothing to do with my resourcefulness or resilience.
For example, euthymic bipolar individuals (euthymia is a stable mental state in those affected by bipolar disorder that’s neither manic nor depressive, yet is distinguishable from healthy controls) were found to have a smaller prefrontal lobe that behaves differently from “normal” during fMRI.
The prefrontal lobe is the seat of higher-order reasoning, decision-making power and risk-taking behaviour in the brain, and this is why you see strong links between addiction and negative health outcomes in bipolar patients.
In manic bipolar patients during fMRI, it was also found that the amygdala (which regulates emotions) wasn’t performing as “normal,” either—which means that you’re out of control, both literally and figuratively.
Off meds vs. on meds
Off meds, I have no baseline or euthymic state. I swing in mood from depression to a mixed state to hypomania, all around and back again. Each state lasts anywhere from three weeks to six months. I’ve even had a depressive phase that lasted for two years.
Why didn’t I get help sooner, you ask? Because I thought my normal was “normal.” I thought that everyone gets depressed from time to time, and was adamant that a pill couldn’t fix it. I wanted to try all-natural remedies. I was very anti-psychiatry.
So what changed? A slew of lost, broken or strained relationships or burned bridges, and a few ultimatums.
My life before medication
 Hypomanic phase
Hypomanic phase
- Expanded self-esteem, delusions of grandeur and increased goal-oriented behaviour
- Increased productivity and creativity; beginning but not completing projects
- Elated mood escalating to frantic; frustration, agitation and aggression and an irritable to raging mood
- Racing thoughts, belligerence, uncontrolled outbursts, the compulsion to over-explain (overly trusting)
- An unintentional and inextinguishable need to express myself—even at the detriment of discretion, professionalism, tact and a true regard for the needs and emotional states of others, or “pressured speech”
- Hypergraphia; excessively distracted by unimportant stimuli; saturated colours and magnified experiences of textures
- Ice-cold and profuse sweats
- Emotional instability during work, play and rest
- Inability to keep track of time
- Insomnia (not sleeping for up to 72 hours at a time)
- Impulsivity and over-indulgence in enjoyable behaviours with a high risk of negative outcomes (shopping compulsively, recreational drug use and such)
- Obsessiveness and intrusiveness
- Hypersexuality
- Abnormal social interaction (markedly increased for me)
- Psychomotor agitation (jaw clenching, leg shaking, foot tapping)
- Reduced appetite and significant weight loss
Depressive phase
- Low mood and aversion to activity
- Rumination and pervasive feelings of sadness, isolation, worthlessness, emptiness, irritability and self-loathing
- Low self-esteem and motivation levels (chronic shyness and social anxiety)
- Hypersomnia
- Zero libido
- Psychomotor retardation, lethargy, and fatigue; aches and pains
- Agoraphobia
- Suicidal ideation
- Comfort eating and drastic weight gain
Mixed state
- Any combination of the above symptoms
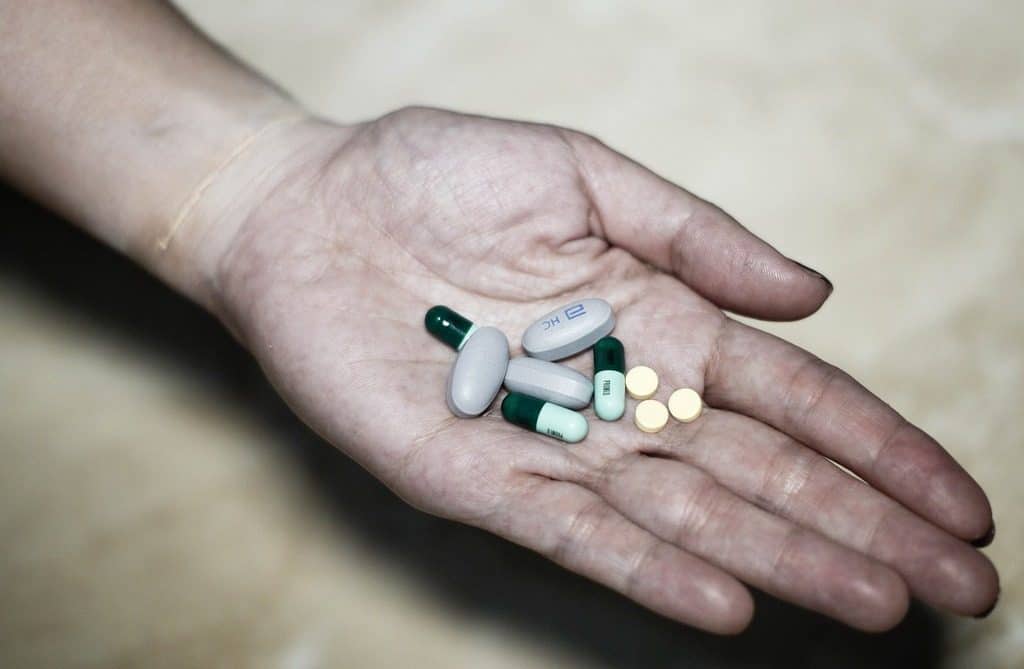 I find mania far more debilitating to my life than depression, but during both phases, I can’t maintain work or relationships for different reasons.
I find mania far more debilitating to my life than depression, but during both phases, I can’t maintain work or relationships for different reasons.
[su_pullquote align=”right”]Because I was so reticent to try medication, it took me about four years from my initial diagnosis to get on my first full cocktail of medications.[/su_pullquote]
When I’m on meds, none of this plagues me. However, this isn’t to say that the medical model of “disease” or “illness” hasn’t failed me.
Because I was so reticent to try medication, it took me about four years from my initial diagnosis to get on my first full cocktail of medications. I stayed on these medications until a medical crisis last year. I was admitted to hospital in October 2017 with renal failure, neuropathic pain and acute illness neuromyopathy due to lithium toxicity, and I wasn’t released until February 2018.
I couldn’t walk. I’m still pretty wobbly. But, despite this, I continue to be a proponent of psychiatric medications because I’ve only been symptom-free while on them.
The upshot
I’m now on a lighter load of medications, and I implement peer support and Yoga into the mix. I feel grounded, self-assured and content in day-to-day life.
The swinging has stopped.
«RELATED READ» FINDING THE ROAD TO HAPPINESS: Advice on dealing with depression while suffering from PMDD/PMS»
[su_panel background=”#f2f2f2″ color=”#000000″ border=”0px none #ffffff” shadow=”0px 0px 0px #ffffff”]Eleanor is an experienced mental health advocate and Peer Support Worker. She facilitates a Narrative Therapy-based writing group every Saturday from 2 to 4 p.m. at St. Joseph’s Heath Centre in Toronto, Canada. For more information, visit mood-mend.com.

